University Place baby undergoes rare surgical procedure mid-birth to save his life
Oliver wanted to breathe the morning of his birth. He tried filling his lungs as doctors held him. But his trachea, obstructed by a malformed airway, couldn’t take in air.
Without intervention, the otherwise healthy boy was destined to die within minutes of his birth Nov. 16 at the University of Washington Medical Center in Seattle. And there wouldn’t be enough time to save him, even with intervention, after he was born.
Fortunately for Oliver, he didn’t need to breathe just yet.
Imaging revealed the birth defect weeks earlier, and doctors were ready. So were Oliver’s parents, Lauren Sanford and Josh Setten of University Place.
“I was sitting on a stool right by her head talking to her, holding her hand,” Setten said of his wife. “We were both listening to what the doctors were saying. And I was trying to do what I could to kind of keep Lauren from getting too overwhelmed.”
For seven minutes on that Tuesday morning, Oliver Setten hovered between being a fetus and a baby, his birth on hold, as a team of 30 surgeons, anesthesiologists, nurses and others worked to give him an airway as he received life-sustaining blood and oxygen from his mother.
The medical team moved, as one doctor later called it, like a well rehearsed orchestra performing a symphony.
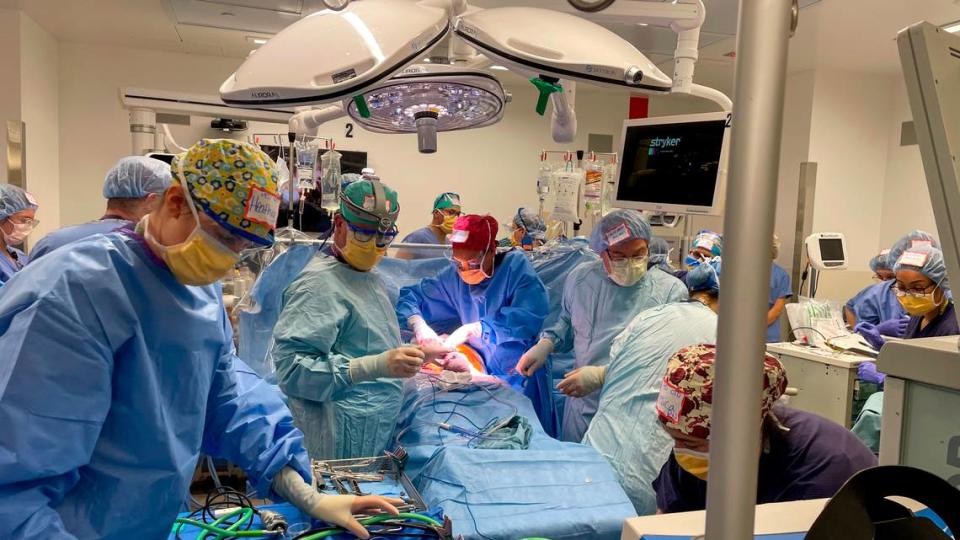
Only when the baby could breathe on his own was the C-section completed and Oliver finished his journey into the world.
The extraordinarily rare procedure, in which a baby’s birth is paused midway for sometimes up to two hours, gets performed just twice a year on average at the UWMC. Called Ex Utero Intrapartum Therapy (EXIT), it allows surgeons to open or repair a baby’s airway while it’s still using the mother’s circulation system to get blood.
The operation carries risks for both the baby and the mother.
For Oliver’s parents, it was the best chance at giving Oliver a long and healthy life.
A normal pregnancy
Oliver is the first child for Sanford, a dance instructor and Setten, a Realtor. Both are 32.
Following a miscarriage in January, the couple wanted to make sure everything that could be checked would be checked with Oliver. Genetic tests came back normal.
At 18 weeks, imaging showed Oliver had a recessed, underdeveloped jaw and cleft palate. The condition is called Pierre Robine sequence. However, Oliver’s tongue was normal. As he developed, his tongue overwhelmed and blocked his airway.
Knowing Oliver’s rare condition needed the most specialized care, the couple’s doctors in Tacoma referred them to UWMC and Seattle Childrens’ Hospital.
Dr. Shani Delaney, an obstetrician who specializes in high-risk pregnancies at UWMC, ordered an MRI.
“No one wants to hear at any point in their pregnancy that something is different with their baby and going to need some special therapy and treatment,” Delaney said.
Oliver couldn’t be operated on in the womb, and his chances for survival were dismal outside of it.
Delaney and other specialists pitched the EXIT Procedure to the couple.
“They all said, you know what, we think that this is probably the safest way to bring your baby into the world,” Sanford said.
Sanford did some online research and was quickly overwhelmed.
“I panicked, because this is way more intense than I was thinking,” she said. Doctors reassured the couple. “They probably walked us through it about 10 different times.”
Not only did the couple have to absorb the news of their son’s condition, they also had to weigh the risks of a complicated birth.
“Our parents are slammed with all of this information that they have to process — the scientific part of it and the medical explanations while they are coping with the super-challenging emotional side,” Delaney said.
Setten took some convincing.
“I was scared,” he said. “I couldn’t stop thinking, ‘Oh, my God, they’re going to cut my wife open.’ It was terrifying.”
The couple tried not to think about all the things that could go wrong.
“Because, if we do that, then we just spiral into fear and anxiety and all those things that is not going to help either me or Lauren or the baby,” Setten said. “And so we just kind of went into it, believing and hoping that everything was going to work out as well as it possibly could, having faith in our doctors and the teams.”
Though the couple weighed their options before agreeing to the procedure there was never any doubt that Oliver came first.
“You’ll do whatever you can to give your child the best shot at life,” Sanford said. “I was holding on to Oliver for dear life.”
EXIT
“We spend a ton of time, prenatally before delivery, really trying to determine who actually needs these,” Delaney said of EXIT procedures. “Just because you can do a procedure doesn’t always mean that you should do a procedure.”
Before anyone sets foot in the operating room, there’s been discussion and coordination between ethicists, radiologists, obstetricians, surgeons, anesthesiologists, neonatologists and nurses.
A woman’s body is not inclined to pause a birth. Whether Cesarean or natural, once the birth process begins, an quick expulsion of the placenta is programmed into the mother’s body.
In an EXIT Procedure, the uterus, in a sense, needs to be tricked that it still has a baby in it and not detach the placenta.
“(EXIT) was initiated so that we could salvage babies who otherwise would not have an airway, after they were separated from mother and they would die,” said Dr. Edith Cheng, a UWMC obstetrician and professor who helped deliver Oliver.
The reasons a baby might not be able to breathe are many: A locked jaw, a lesion or tumor that has blocked the airway, neurological problems. All of them can be corrected or at least lessened with surgery, intubation or other methods.
Sometimes the procedures take much longer than the few minutes a baby can go without oxygen. In those cases, the baby dies.
Cheng performed her first EXIT in 2010, just a few years after other institutions started performing them. UWMC and Seattle Children’s are the only providers of the procedure in the Pacific Northwest.
While the reasons for an EXIT vary along with the remedies, the process that keeps babies alive for those crucial minutes is the same: staying attached to a functioning placenta. It acts as a heart and lung machine for the baby, Cheng said.
The longest a baby and mother have had to stay in this suspended state of birth at UWMC is two hours, Cheng said.
The operation takes so many people because separate teams are needed to monitor and assist both the mother and baby.
In Oliver’s case and by design, only his head and one arm emerged from his mother’s uterus. An anesthesiologist put an IV into his arm to administer drugs to relax him.
Oliver was trying to become a baby, she said, and doctors needed him to stay a fetus a little bit longer.
Welcome to the world
Oliver’s original due date was Nov. 30. Doctors decided to deliver him at 38 weeks to make sure Sanford didn’t go into labor early.
As soon as Oliver was partially removed from the uterus, a doctor held onto his neck to keep it stable. Then, a team of pediatric surgeons took over.
“And then the pediatric (ear, nose and throat) people start putting a scope in the baby’s mouth to look around and see if we can intubate,” Cheng said.
Once Oliver was intubated through his nose and could breathe, Cheng and her colleagues clamped and cut the umbilical cord.
He weighed 7 pounds, 7 ounces and was 18.9 inches long.
“When we saw him be transferred from her to the table where they were going to work on him, we both started crying,” Setten said. “And they were saying he was healthy and everything worked.”
“This was my first surgery ever, and I pretty much had the Mount Everest of surgeries,” Sanford said.
Setten now had a family to look after.
“I was torn between going with my new son and staying with my wife who was still dealing with this major surgery,” he said.
Oliver was soon transferred to Seattle Children’s Hospital.
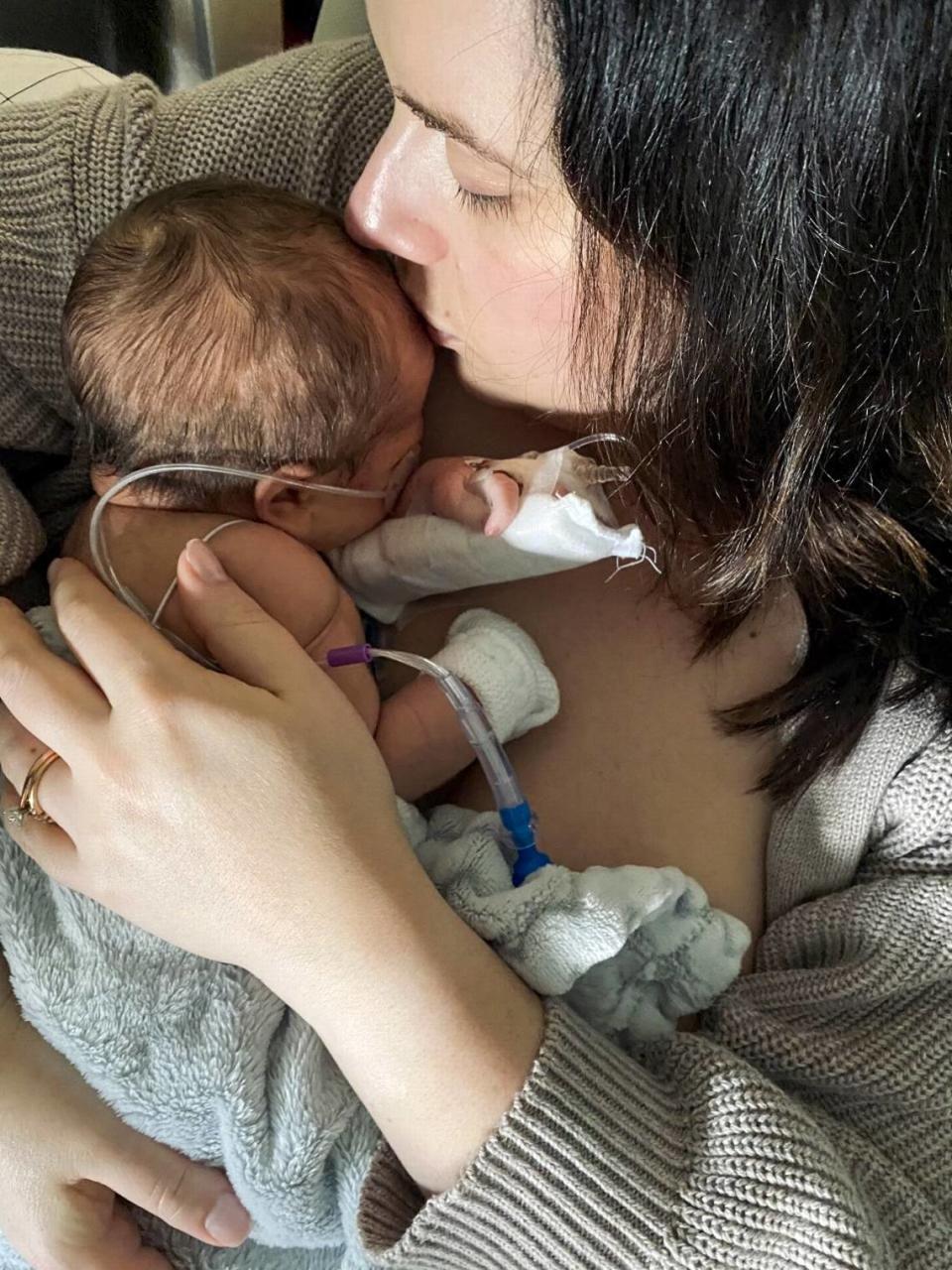
In the immediate days after the birth, the couple wasn’t able to hold their son. He had too many wires, tubes and other devices attached to him. But they were able to touch his face and rub his arms.
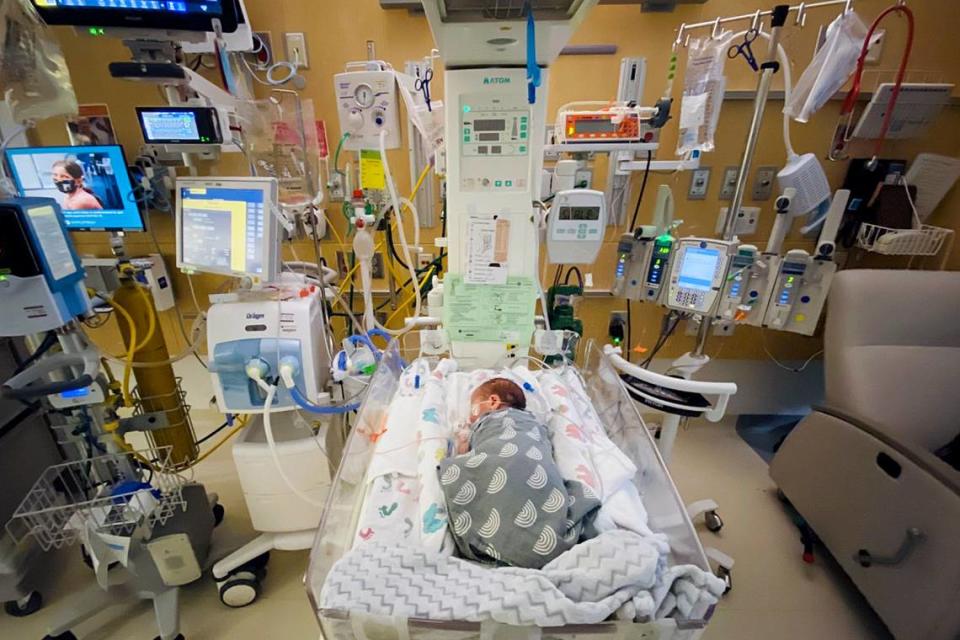
The couple don’t know when they’ll be able to take him home to University Place.
“Initially, they said that he could be in the hospital anywhere between two weeks and a year,” Setten said.
Two days after his birth, Oliver’s intubation tube was replaced with a cannula tube which can more precisely regulate his oxygen supply.
Further imaging this week showed that Oliver will most likely need surgery to lengthen his jaw and open his airway. The couple have been able to change his diapers, bathe him and hold him.
“We’re very much a part of his care,” Sanford said.
For Delaney, who was in the operating room that day, births like Oliver’s are stressful.
“They’re also some of my favorite cases, just in terms of, this is why we do what we do,” she said. “And I’m so happy that we can help babies like Oliver and help their parents through one of the most challenging parts of their life.”

 Yahoo Autos
Yahoo Autos 