Will the US face another bad COVID-19 winter? Cases are falling, but the virus isn't done with us, experts say
COVID-19 rates are finally falling again after a wave nearly as bad as the one last winter. Hopefully, we are through the worst of the pandemic.
But experts warn that if we start acting as if COVID-19 is over, we definitely won't be.
Behavior has a major impact on what happens with the virus, and if people stop taking precautions, start gathering in large numbers and not getting vaccines or boosters, another wave could strike this winter.
“A lot of it depends on human behavior, and human behavior in this pandemic hasn’t served us very well,” CDC director Dr. Rochelle Walensky said in a recent call with reporters. “We are battling with ourselves, not with the common foe.”
The virus that causes COVID-19 thrives in cool, dry air. And when people gather indoors, especially unmasked, they are more likely to transmit it.
The holidays are coming, and travel and large gatherings serve as viral breeding grounds.
For many people, vaccinated or infected months ago, protection against the virus that causes COVID-19 may be waning.
Still, there are positive signs that America's pandemic could get better rather than worse over the next few months.
COVID-19 infection rates fell about 12% last week compared with the week before, and hospitalizations dropped 14%, Walensky said in a news conference.
Vaccines for kids ages 5-11 are expected to become available in about three weeks. Although children are less likely to suffer severe consequences from the virus than older adults, they can get very sick and can pass the virus on to others. Vaccinating large numbers will help slow the virus' spread.
In some areas, vaccination rates are so high that, combined with natural infections, it could be hard for the virus to gain a foothold among the relatively few people left unprotected.
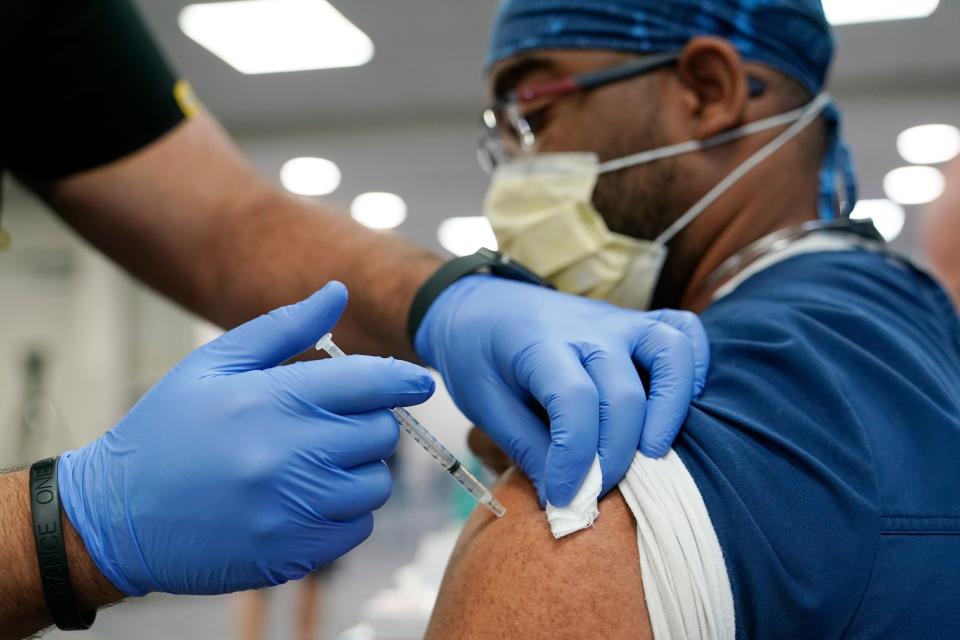
Boosters are becoming widely available, renewing protection for the immunocompromised and those who got the Pfizer-BioNTech vaccine and who are also over 65, at high risk for serious disease or in particularly vulnerable professions. This week, federal agencies will begin the process of examining and likely authorizing boosters for the other two available vaccines.
New treatments coming online soon, including an antiviral pill, should cut down on the number of people who need hospital care and are at risk of death, easing the strain on hospitals and health care workers.
And rapid, cheap testing is finally getting ramped up, well over a year after experts began calling for wider availability of coronavirus tests.
The pandemic "is not magically over," said Dr. Kirsten Bibbins-Domingo, chair of the department of epidemiology at the University of California, San Francisco. But the "worst does look like it's behind us."
The SARS-CoV-2 virus has been unpredictable for nearly two years now, though, and it's likely to remain part of our lives forever.
"If we proceed in the way we have in the past without additional cautions in place, that virus will eventually find the vulnerable amongst us and will wreak havoc," Bibbins-Domingo said. "This is what this virus has shown it is very capable of doing."
Learning to live with COVID-19
The virus has spread so far and so fast, it doesn't seem possible anymore to eradicate it, experts say. Instead, we will eventually reach an uneasy peace, as we have with the flu and common cold, where infections might spike occasionally in certain areas, but most people will be protected from serious disease.
Getting more people vaccinated will help us reach that milestone, said Warner Greene, a virus expert at Gladstone Institute in San Francisco.
"This virus will continue to circle back and prey upon us until we can get much higher vaccination rates," he said.
So far, about 56% of the total U.S. population is fully vaccinated, according to the CDC.
Unfortunately, as with the cold and flu, it seems this virus can be caught over and over again, as natural infection and protection from shots fade over time.
What's not entirely clear yet is whether subsequent infections are less dangerous than initial ones. While most "breakthrough" cases after vaccination don't require hospitalization, some still do, and it's not known whether a second natural infection will be less severe than a first, Greene said.
The virus isn't done with us, said Jeffrey Shaman, an infectious disease epidemiologist at Columbia University's Mailman School of Public Health.
Delta has definitely changed the course of COVID-19, Shaman said, turning what looked to be the end phase of the U.S. pandemic into the start of a new wave.
It's not entirely clear how new variants emerge, Shaman said. It could be because the virus changes as it passes from person to person, or variants could breed in immunocompromised people whose immune systems can't quite tamp down the virus. "Do you need a lot of people or just the right people?" he asked, adding that researchers aren't certain.
Shaman said he understands it's hard for the public to remain vigilant about something they can't see.
"Nobody every witnesses the actual transmission of virus," he said.
At least for now, COVID-19 remains far deadlier than the flu. Even in the last flu pandemic, the H1N1 pandemic of 2009-2010, about 76 out of every million people who caught it died. With COVID, he said, 3,000 out of every million people infected will die.
If natural infections, vaccines and better treatments can cut that death rate, it will become easier to live with COVID-19, Shaman said.
With new strains of the flu, it usually takes a year or two for the virus to settle into a steady state, with just one winter wave rather than repeated ups and downs, said Lauren Ancel Meyers, a professor of biology and statistics at The University of Texas at Austin.
"Two winters from now, will COVID have settled into a seasonal dynamic where it tends to lay low in summers and we have a wave or two in the winter? That's very plausible," Meyers said.
But it's too soon to say whether that pattern will appear this winter, she said. She hopes people will be prepared to mask up again if they start seeing an increase in cases. It makes sense to add layers of caution when cases start to rise, and relax behaviors when they drop.
"At every turn, this virus demands new kinds of responses from us," she said. "We have to stay on our guard."
Looking ahead
Bibbins-Domingo said people like her are often portrayed as as "doomsayers," but she thinks it's within the public's power to prevent another wave of infections and deaths.
"If we move cautiously in the next period, we can get through the winter months fine," she said.
Bibbins-Domingo said she'd like to avoid the "whiplash of going 'everything is great, take everything off,' to 'oh my gosh, the hospitals are full again.'"
A range of forecasting models suggest things will get better going forward, said Nicholas Reich, an expert in biostatistics and infectious disease epidemiology at the University of Massachusetts, Amherst. He's encouraged by the fact they're all trending in the same direction.
"The general sense in the data right now and in the models, too, is one of guarded optimism," he said. "That feels like a reasonable place to be in."
While the nation as a whole may be through the worst of the pandemic, some unlucky pockets could still be hard-hit, said Stephen Kissler, a postdoctoral research fellow at the Harvard T.H. Chan School of Public Health.
"We're not out of the woods, but I really don't think especially in terms of deaths and hospitalization we'll see the sort of thing we saw last winter," Kissler said. With such a large percentage of people having been infected or vaccinated, "I don't think cases will translate nearly as much into deaths this winter, thankfully."

The future also depends on whether the virus, which as Shaman said, has been "squirrelly" so far, manages to throw another curveball.
Kissler said he's not as worried about variants as he was a few months ago. Delta is so contagious, he said, that it seems to have crowded out other variants, making it hard for them to gain a foothold.
"Delta has been winning out," in competition with other variants, he said. "I'm cautiously optimistic that we'll be dealing with delta and only delta."
A new variant could impact areas differently, depending on how it behaves, Reich said. In Vermont, where vaccination rates are high but not many people have caught the virus, a variant that escapes the vaccine but not natural infection might chart a different path than in places like Arizona and Florida, where vaccination rates are lower but a much higher percentage of residents have been infected, he said.
Of course, what happens in the United States is only part of the story. If the virus continues to rage in other parts of the world, that will increase the chances of more infections and the emergence of new, more dangerous variants.
Said Norman Baylor, a vaccine expert and president and CEO of Biologics Consulting: "We're not close to the endgame until the world is close to the endgame. Period. Full stop."
Contact Karen Weintraub at kweintraub@usatoday.com.
Health and patient safety coverage at USA TODAY is made possible in part by a grant from the Masimo Foundation for Ethics, Innovation and Competition in Healthcare. The Masimo Foundation does not provide editorial input.
This article originally appeared on USA TODAY: The end of COVID in the US depends on behavior and the uncertain virus

 Yahoo Autos
Yahoo Autos 